The term “babies with drug addiction” refers to newborns who are exposed to drugs or certain medications during pregnancy. Babies do not consume these substances voluntarily; they pass from the mother’s bloodstream to the fetus through the placenta, and the baby becomes accustomed to these substances.
After birth, drug intake is abruptly cut off, and the baby is deprived of the substance it is dependent on, beginning to show withdrawal symptoms: loud crying, trembling, sleep or feeding problems, diarrhea, fever... This condition is known as Neonatal Withdrawal Syndrome (NWS) and can range from mild forms to complex situations; complex cases may require treatment in neonatal intensive care.
What is Neonatal Withdrawal Syndrome?
Neonatal Withdrawal Syndrome is a series of symptoms that occur in the first days or weeks after birth when the fetus has been exposed to addictive substances. The most common are opioid substances (heroin, methadone, morphine, codeine, oxycodone...), but it can also be seen with other drugs (cannabis, cocaine, amphetamines, alcohol, benzodiazepines, barbiturates, and some antidepressants).
These substances can cross the placenta barrier, so everything present in the mother’s blood can reach the fetus’s blood. If substance use continues, the baby becomes accustomed to living with these substances. When born, if drug intake is suddenly stopped, the nervous system becomes unstable, and the typical “withdrawal crisis” occurs.
A frequently mentioned type within NWS is neonatal opioid withdrawal syndrome; this occurs when the affected substance is an opioid (heroin, methadone, morphine, fentanyl, etc.). In these cases, symptoms are usually more intense and can persist for a longer time.
Not all cases are related to illegal substance use; many mothers have taken opioid medications prescribed by healthcare professionals as part of intensive pain management or heroin addiction recovery programs. However, the baby can still develop withdrawal syndrome after birth.
Main Causes: Related Drugs and Medications
NWS can arise after exposure to almost any substance that affects the central nervous system. The more drugs used (polydrug use), the higher the risk and severity of symptoms. The most studied substances include:
Opioids are the primary causes of neonatal withdrawal syndrome. This group includes heroin, opium, methadone, morphine, codeine, and other medical opioid analgesics (such as oxycodone, hydrocodone, meperidine, or fentanyl). Continuous exposure during pregnancy can lead to significant withdrawal in the newborn; in this case, symptoms such as trembling, loud crying, digestive issues, and excessive irritability may be observed.
Benzodiazepines and hypnotic-sedatives (diazepam, lorazepam, alprazolam, bromazepam, etc.) can also trigger withdrawal if the mother has taken these medications for a long time. Here, the blood levels at the time of birth and the total exposure duration are important. Abrupt cessation of drug transfer can cause the baby to experience trembling, sleep difficulties, changes in muscle tone, and autonomic instability.
In the case of cocaine, rather than a classic withdrawal syndrome, direct toxic effects on the developing brain are observed. These newborns are often very irritable, trembling, loudly crying, and experiencing sleep and feeding problems. Additionally, it increases the risk of placental abruption, preterm birth, and low birth weight during pregnancy.
Amphetamines and methamphetamines (speed, crystal, etc.) are associated with fetal growth restriction (low weight, height, and head circumference) and are related to irritability, hypertonicity, and feeding problems after birth. Although the symptoms can be striking, they can often be treated without requiring large doses of medication, but this condition may later affect neurodevelopment.
Cannabis is commonly thought to have no effects, but evidence shows higher risks such as low birth weight, heart abnormalities, and excessive arousal issues in newborns. These babies may experience tremors, frequent waking, and sleep problems. Prenatal cannabis exposure has been associated with long-term learning and behavioral issues.
Alcohol has its own section related to fetal alcohol spectrum disorders. Here, not only is there an acute postpartum picture, but also a structural impact on development: very slow growth during and after pregnancy, characteristic facial features, heart abnormalities, and significant delays in cognitive development. The clinical picture associated with alcohol consumption can last up to a year and a half in some cases.
Tobacco should not be overlooked either. Smoking during pregnancy is associated with low birth weight, premature birth, fetal death, sudden infant death syndrome, and ongoing respiratory and neurological complications in childhood. Nicotine, like any psychoactive substance, also affects the baby's nervous system.
Additionally, some SSRIs antidepressants or barbiturates, and less studied drugs (such as MDMA or LSD) can also be effective. In the case of MDMA, it has been observed that babies whose mothers used this substance may show worse coordination and slower movements by four months, but there is no significant withdrawal syndrome.
How and When Do Symptoms Appear in the Baby?
How NAS appears depends on several factors: type of substance, dose, duration of use, time of last use, gestational age of the baby (whether born prematurely or on time), and the situation of multiple exposures. Therefore, the two pictures are not exactly the same.
Withdrawal symptoms in many newborns appear 24 to 72 hours after birth, but in some cases, they can be delayed by 5-10 days; this is especially true for substances with a long half-life or for benzodiazepines and methadone. In cases of opioid exposure, subacute symptoms can last up to six months in some instances.
The most common symptoms in babies born on time include tremors, continuous and loud crying, difficulty falling asleep, increased muscle tone (hypertonia), exaggerated reflexes, frequent yawning, sneezing, nasal congestion, difficulty coordinating sucking and swallowing, vomiting, diarrhea, sweating, fever, or unstable temperature.
Many babies with NAS experience serious challenges with feeding and weight gain. They often prefer biting instead of sucking, tire quickly during breastfeeding or bottle feeding, and struggle to coordinate breathing and sucking. This leads to slow weight gain and a need for more monitoring by the neonatal team.
In the most severe cases, the baby may experience seizures, accelerated breathing, and significant dysregulation of the autonomic nervous system; in this case, intense sweating, tachycardia, and fever episodes may be observed. Skin spots or irritations may be seen, and digestive issues (watery stools or recurrent vomiting) frequently arise.
Premature babies interestingly sometimes show less pronounced or shorter-lasting symptoms; this is because they have been exposed for a shorter time in utero. However, this does not mean that the drug has no effect on development; in fact, the risk of prematurity combines with the potential consequences of exposure to toxic substances.
Diagnosis: How is “Withdrawal” Confirmed in a Baby?
The diagnosis of NAS is primarily based on two key elements: on one hand, the mother's history of drug or medication use, and on the other hand, the symptoms exhibited by the newborn in the first days of life. It is important to conduct an in-depth clinical interview in a safe environment to clarify what types of substances the mother has used, for how long, and in what amounts.
Obtaining this information is not always easy. Many women experience feelings of guilt and fear of judgment or may deny substance use due to fears of losing custody of their children. Therefore, if the clinical picture raises suspicion, professionals may resort to special analysis tests.
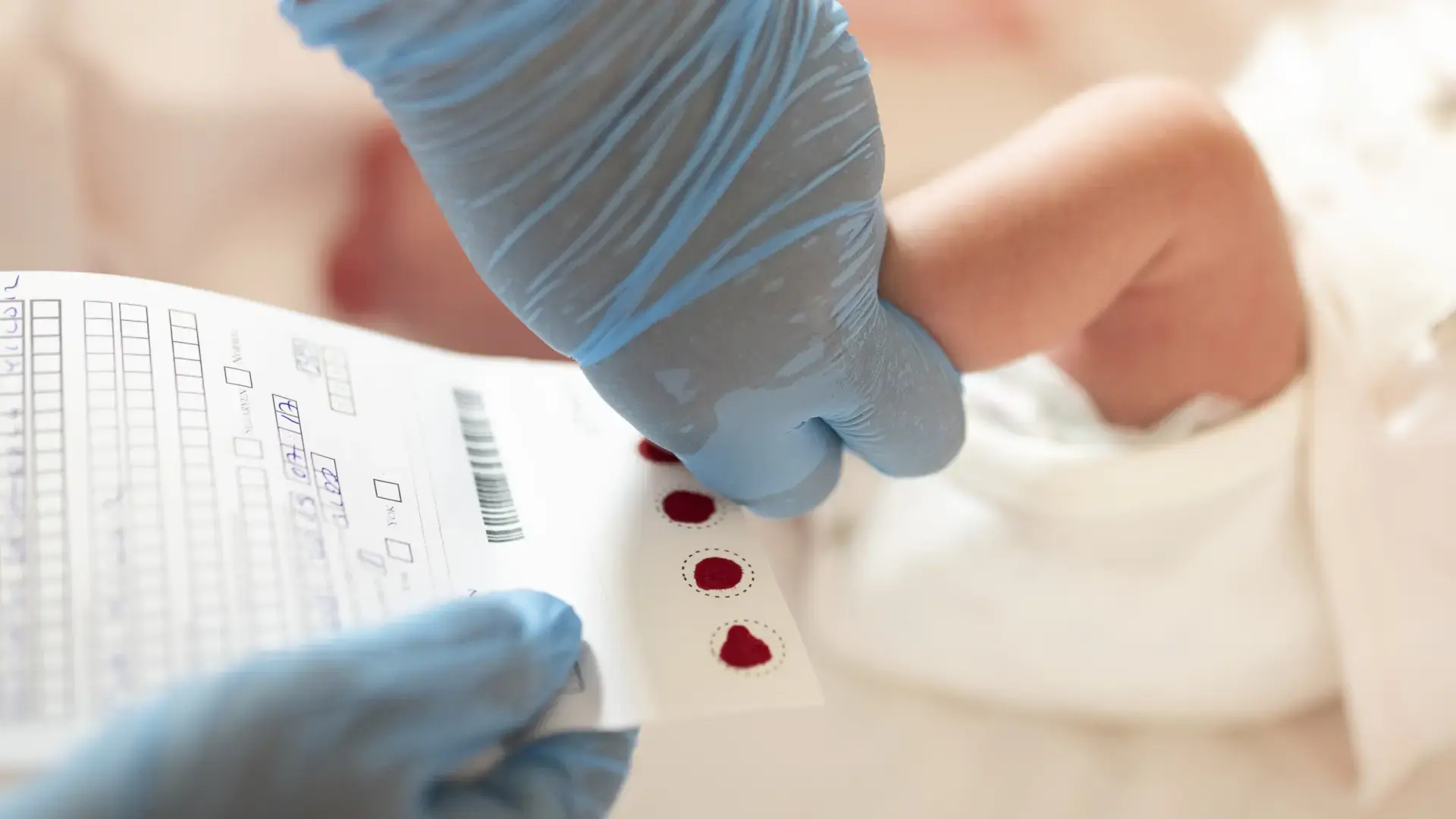
Among the tests performed are baby urine, blood or meconium analysis (the first stool passed after birth) and even umbilical cord tissue analysis. These tests help detect the presence of various drugs and confirm intrauterine exposure; this is possible even if it occurred days or weeks before birth.
Standardized scoring systems are used to assess the severity of the syndrome. Traditionally, scales have been used that collect scores based on the severity of symptoms such as crying, tremors, muscle tone, digestive issues, or sleep patterns. More recently, the ESC scale (“Eating, Sleeping, Soothing”) has become common; this scale evaluates three essential aspects of the newborn.
The ESC approach assesses whether the baby is being fed appropriately (eating), whether they are sleeping for the minimum age-appropriate duration (sleep), and whether they are calming down with usual soothing strategies (soothing). If the situation in these three areas is reasonably controlled, supportive measures may often be sufficient without medication.
Hospital Treatment: From Physical Comfort to Medications
Once NYS is identified, treatment is tailored to the baby's condition and includes a combination of environmental care, family support, and medication when necessary. The goal is not only to alleviate acute discomfort but also to minimize the impact of withdrawal on growth and early development.
The first step in treatment is to create a comfortable and regular environment. Newborns are usually kept in rooms with low light and noise; thus, stimuli that could disturb them are minimized. Methods such as swaddling with a not-too-tight blanket, gentle rocking, and providing skin contact (kangaroo style) are used to help reduce irritability.
The role of families is very important. They are encouraged to spend as much time as possible with their children; holding their baby, maintaining good contact, speaking in a gentle voice, singing, and actively participating in their care is essential. This continuous support helps the baby to calm down, reduces the need for medication, and shortens the hospital stay.
In terms of nutrition, many newborns with NYS are seen to need extra calorie intake; as they expend more energy due to tremors, crying, and difficulty sleeping. Sometimes feeding is preferred more frequently but in smaller amounts, allowing the babies to take breaks to avoid becoming fatigued. In cases of severe vomiting or diarrhea, the baby may need to be fed intravenously.
When relaxation measures are insufficient and symptoms are very severe, replacement therapy is applied. A medication similar to the substance causing addiction (for example, oral morphine or methadone in cases of opioid exposure) is usually used; this medication is given in controlled doses and gradually reduced, thus managing withdrawal symptoms.
Other medications such as subcutaneous buprenorphine, clonidine, or phenobarbital are used for specific situations. While clonidine can help reduce heart rate and decrease autonomic hyperactivity, phenobarbital is often used to control seizures or in babies exposed to cocaine or cannabis. All this treatment is carried out under very strict supervision in specialized neonatal units.
The process of discontinuing medications can take from days to several weeks, depending on the severity of the syndrome and the baby's response. During this time, the health team reassesses the withdrawal score daily and adjusts the dosage to ensure that symptoms remain at a manageable level; this is done without intense pain or excessive sedation.
How Can Families Help Their Babies?
Families are not just spectators in the process; they are an active part of the treatment. Babies with NYS require more care, more patience, and more contact than other newborns. Therefore, it is very important for mothers, fathers, or other caregivers to receive clear guidance and emotional support from the very beginning.
It is recommended that the child be kept in a calm, low-light environment away from sudden stimuli at home and in the hospital. Always sleeping on their back on a firm and safe surface reduces the risk of sudden infant death. When swaddling the baby, care should be taken not to make the blanket too tight; it should not restrict their movements or breathing.
Other helpful strategies include frequently applying skin-to-skin contact, keeping the baby close to the body, gently rocking (without harsh jolts or overly stimulating touches), offering a pacifier when there is a need to suck, and accompanying with soft music, humming, or a calm voice. All of these contribute to the baby feeling secure and lowering the level of stimulation.
Feeding should be done in as calm an environment as possible, away from noise and distractions; the baby's rhythm should be respected. Breastfeeding can be a valuable tool for mothers on treatment programs controlled by methadone or other opioids; in this case, it should be ensured that no other drugs are actively used. Breast milk can reduce the severity of some withdrawal symptoms and promote bonding.
Diaper changes should be done frequently, keeping the area clean and dry, and monitoring for any irritation or rashes on the skin. If the baby is sucking their fingers excessively, it is important to offer them a pacifier, keep their hands clean, and use gloves if necessary to prevent them from scratching their face. In case of nasal congestion, gently clearing nasal discharge with saline solution and keeping the child in a more upright position while awake is sufficient.
There is an important message that experts repeatedly emphasize: the baby should never be shaken. If at any point the situation overwhelms the caregivers and they lose their patience, the most sensible thing to do is to place the baby in a safe place (crib or bassinet) and take a few minutes to breathe or seek help from a trusted person.
Short and Long-Term Complications and Outcomes
In addition to the difficult times the newborn experiences during withdrawal, drug use during pregnancy can lead to many medical complications. These include low birth weight, congenital abnormalities, microcephaly (smaller than normal head), jaundice, respiratory and circulatory issues, or even fetal death and respiratory failure at birth.
Exposure to cocaine, amphetamines, or cannabis has been associated with learning difficulties, attention disorders, and impulsivity during childhood; it also increases the risk of low IQ and behavioral disorders. The environment in which these children grow up (economic resources, family stability, school support, etc.) can further exacerbate or alleviate these issues.
Follow-up studies, such as one conducted in Australia, show that children born with NAS are twice as likely to repeat a grade in school compared to their unexposed peers. Additionally, hyperactivity, deficiencies in motor skills, verbal memory issues, anxiety, depression, and increased risk of substance use in adolescence are observed.
In the case of alcohol, fetal alcohol spectrum disorders are often associated with overall developmental delays; this can leave a lasting impact on cognitive, social, and autonomy skills. These children may require long-term follow-up with special education support, stimulation therapies, and pediatric neurology and child mental health teams.
In many infants, the withdrawal syndrome may resolve within a few days or weeks and improve acceptably; however, the reality is that issues should not be closed at discharge from the hospital. Close coordination among pediatricians, social service specialists, psychologists, and addiction services is essential; this is important to support the family, prevent mothers from becoming re-dependent, and ensure that the child receives appropriate care and stimulation in their daily life.
Is It Possible to Prevent a Baby's "Withdrawal" Condition?
The only real way to prevent NAS is for the woman to not use drugs or certain risky medications before or during pregnancy; or to do so only under close medical supervision and with clear recommendations. There is no safe amount of alcohol, cannabis, cocaine, or tobacco during pregnancy; any consumption can lead to consequences to varying degrees.
Experts recommend that those who use substances and wish to become pregnant use effective birth control methods; thus, the fetus will not be affected until treatment for addiction begins. If pregnancy is already ongoing and the woman is taking opioids, benzodiazepines, or other substances, she should never stop suddenly on her own. Sudden withdrawal can lead to serious complications for both the mother and the baby. In these cases, the most sensible thing to do is to speak with a healthcare professional as soon as possible and prepare an intervention plan; this plan may include medication-assisted treatment (such as methadone programs) and psychological support.
In many countries, there is a network of specialized resources for pregnant women with addiction issues; these resources combine obstetric care, social support, and addiction treatment. Additionally, there are anonymous and free helplines available to refer to specialized services. The important thing is for the future mother to know that she is not alone and that asking for help is an act of responsibility for both her baby and herself.
With good information, close professional support, and active family involvement, many babies exposed to substances during pregnancy can overcome withdrawal syndrome and develop in a much more positive way than expected. The key is to take action early, reduce consumption as much as possible during pregnancy, and provide a stable, loving, and good care environment for the newborn from day one.



































Comments
(9 Comments)