The well-known heel prick test is a procedure performed on newborn babies within a few days of birth using a small needle, marking an important step in the National Health Service. The Ministry of Health has approved the expansion of the newborn screening portfolio, which includes 21 diseases that must be detected in all public hospitals.
With this update, the test is becoming a wider preventive tool, moving beyond focusing solely on a few classic metabolic diseases. This includes rare but serious disorders and diseases that can be treated if diagnosed in time. Additionally, this measure aims to ensure equity of access and that the inclusiveness of screenings is not dependent on postal codes.
What is the heel prick test and why is it being expanded to 21 diseases?
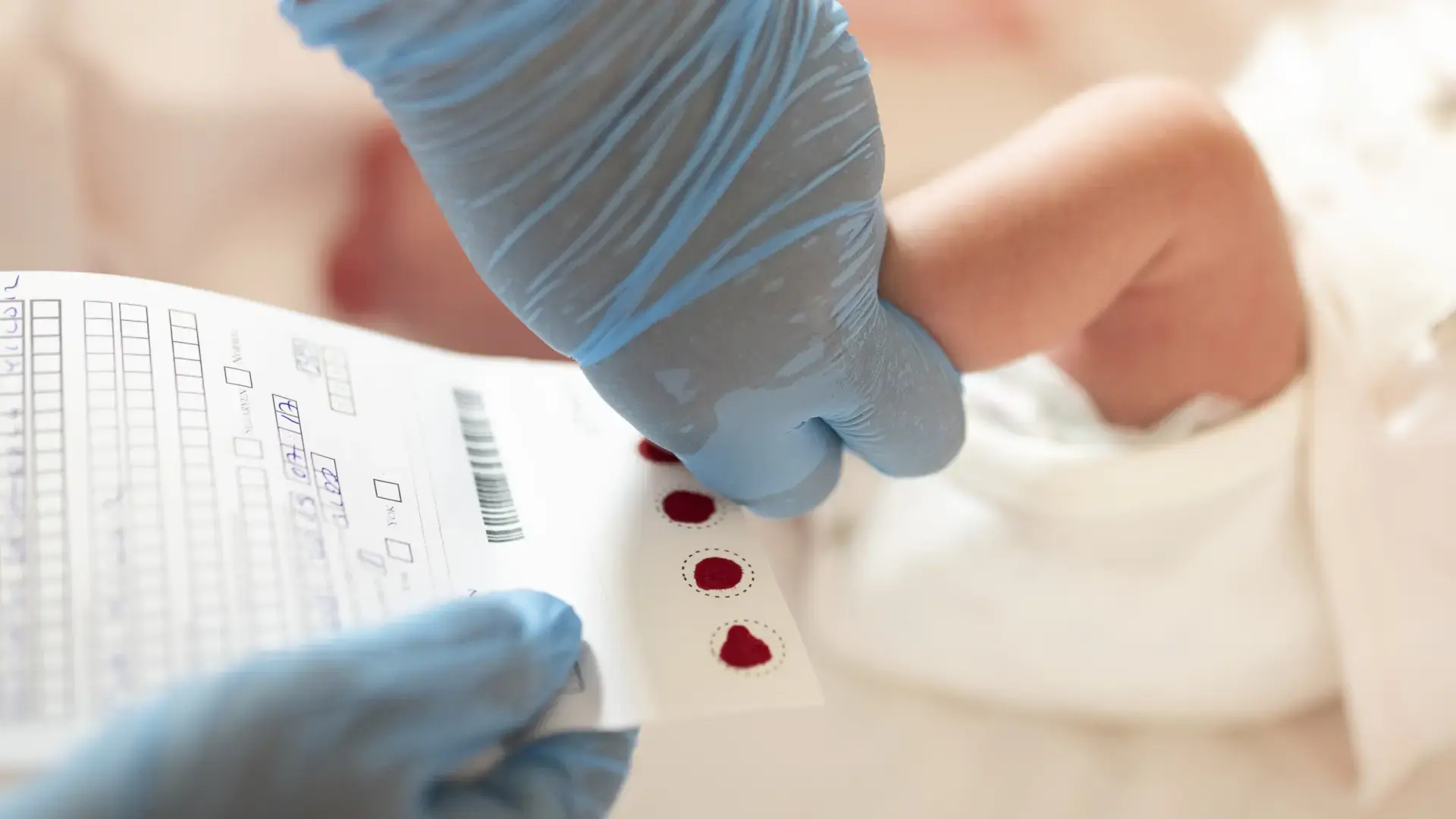
The heel prick test is a newborn screening that involves collecting drops of blood from the heels of newborns and is typically performed between 24 to 72 hours of their lives. This small blood sample allows for the analysis of the presence of certain congenital diseases, most of which are related to metabolism or the function of major glands and organs.
So far, the number of diseases that had to be included in the shared portfolio of services of the National Health Service had gradually increased, but there were significant differences among autonomous regions. While some regions offered a very broad screening panel, others were limited to almost the legal minimum, creating a noticeable sense of inequality among families.
The Ministry of Health had increased the number of diseases that all regions must detect to between seven and eleven. Now, with the new regulation published in the Official State Bulletin (BOE), a qualitative leap is occurring: the heel prick test will have to cover 21 congenital diseases nationwide.
The rationale for this decision is based on several areas: on one hand, advances in laboratory techniques offer the possibility of analyzing more diseases with the same blood sample; on the other hand, there is evidence that these screenings reduce serious complications, disabilities, and deaths with early intervention. Additionally, the desire to strengthen prevention stands out as a central pillar of public health.
Diseases previously included in newborn screening
Before this expansion, the national newborn screening program covered a range of diseases that were integrated by nearly all regions. Among these, there are several diseases considered "classic" in early diagnosis programs.
The list of diseases previously included in the shared portfolio of services consisted of:
- Congenital hypothyroidism, a thyroid gland disorder that can cause delays in physical and cognitive development if left untreated.
- Phenylketonuria, a metabolic disorder that cannot properly process phenylalanine and can harm the central nervous system if not controlled by diet.
- Cystic fibrosis, a genetic disease primarily affecting the lungs and pancreas, requiring early intervention to improve quality of life and lifespan.
- Medium-chain acyl-CoA dehydrogenase deficiency (MCADD), a problem in fat metabolism that can lead to severe hypoglycemic attacks.
- Long-chain 3-hydroxy acyl-CoA dehydrogenase deficiency (LCHADD), another disorder in the beta-oxidation of fatty acids that carries a risk of metabolic imbalance.
- Glutaric acidemia type I (GA-I), which affects the metabolism of certain amino acids and can lead to neurological damage if not prevented.
- Sickle cell anemia, an inherited hemoglobinopathy that causes deformities in the shape of red blood cells, leading to painful crises and organ complications.
These diseases have become established within the clinical practice of newborn screening, and it has been proven that detecting them in the first days of life makes a significant difference: this allows for the initiation of diet, medication, or special follow-up treatment before the symptoms of the disease worsen.
Nine new diseases added to the heel test
The biggest innovation of the update is the increase in the number of screenings added to the heel test from 12 to 21. Most of these are rare metabolic diseases that can result in serious conditions, pediatric intensive care admissions, or even loss of life if not diagnosed early.
The Ministry of Health states that, along with the previously mentioned diseases, the following diseases will also be included in the heel test:
- Biotinidase deficiency (DB) prevents the reuse of biotin (vitamin B7) and, if untreated, can lead to seizures, skin problems, and developmental delays.
- Maple syrup urine disease (MSUD) is a serious disorder in the metabolism of branched-chain amino acids.
- Homocystinuria affects the metabolism of methionine and can be associated with disorders in blood vessels, bones, and eyes.
- Congenital adrenal hyperplasia (CAH) is a group of disorders affecting hormone production in the adrenal glands.
- Tyrosinemia type I (TYR I) is a disease that affects tyrosine metabolism and can damage the liver and kidneys if not diagnosed in time.
- Propionic acidemia is a congenital metabolic defect that causes the accumulation of organic acids and can lead to serious metabolic imbalances.
- Primary carnitine deficiency complicates the transport of fatty acids to the mitochondria and carries the risk of heart failure or hypoglycemia.
- Long-chain acyl-CoA dehydrogenase deficiency is a lipid metabolism disorder that has now been systematically included.
- Methylmalonic acidemia in its various forms: isolated methylmalonic acidemia and homocystinuria with methylmalonic acidemia, as well as isovaleric acidemia, all of which can lead to potentially fatal metabolic crises if not diagnosed early.
This group of metabolic diseases also includes a disease of great importance in pediatrics: severe combined immunodeficiency, a profound immune system disorder that leaves infants almost defenseless against common infections. Early diagnosis facilitates measures such as isolation, specific vaccinations, and even stem cell transplantation.
Official documents and additional explanations also refer to the inclusion of diseases such as spinal muscular atrophy, 3-hydroxy-3-methylglutaric aciduria, or X-linked adrenoleukodystrophy in certain regions. Although the implementation may be gradual, the overall trend is to consolidate around at least 21 diseases for the national panel and to remain open to future expansions based on scientific evidence.
An important program to reduce social inequalities
One of the most important points emphasized by the Ministry of Health is the goal of eliminating the differences between heel tests. So far, some regions have been ahead by voluntarily including many of these diseases in their panels, while others have remained at the mandatory minimum.
This situation created a sense of "geographic lottery" for families; depending on the birthplace of their babies, they could access a very comprehensive early diagnosis program or a much more limited program. With the new regulation, a common ground for 21 diseases has been established that all autonomous regions must guarantee within public health.
The text also states that regions will have a period to adapt their laboratory infrastructure, organize the flow of healthcare services, and ensure the fastest possible delivery of heel test results. The aim is for the expansion not to remain just on paper but to reflect effective changes in daily clinical practice.
The update of the heel test is part of a broader vision for early diagnosis and prevention in Spain, being considered as one of the strategic pillars in newborn screening and child protection. This aims not only to save lives but also to prevent years of suffering, frequent hospitalizations, and very high health and social costs.
Impact on families and the healthcare system
For families, the expansion of the heel test means more peace of mind, especially during the vulnerable postpartum period. No one wants their child to have a congenital disease, but the existence of a comprehensive screening program minimizes the risk of a serious illness going undetected for weeks or months.
Clinically, pediatricians and metabolism specialists emphasize that most of these diseases are silent at birth: a baby may appear completely healthy, but if the underlying issue is not detected, it can develop into a critical condition within hours or days. When the results of the heel test are communicated quickly, it allows for adjustments in nutrition, medication, or care before symptoms appear.
From a public health perspective, various studies show that while these newborn screening programs initially require investment in equipment and training, they are cost-effective in the medium and long term. Preventing serious disability or multi-organ failure not only improves the quality of life for the patient and their surroundings but also reduces the need for long-term hospitalizations, complex interventions, and high-cost chronic treatment requirements.
Increasing the number of diseases included in the heel test to 21 is therefore aligned with a national strategy that prioritizes early access to health issues. The new legal framework also opens the door to future expansions as long as there is sufficient evidence of the benefits of screening and laboratory systems can guarantee to undertake it safely and with quality.
With this reform, the heel test is becoming one of the strongest tools for protecting child health in public health, offering a broader, balanced across regions, and consistent diagnostic coverage with proposals and trends observed in other European countries for newborns in Spain.

































Comments
(9 Comments)