Scarlet fever, also known as “scarlet fever”, is a highly contagious disease caused by group A streptococcus bacteria (Streptococcus pyogenes). This disease is most commonly seen in children aged 2 to 15 years (rarely seen in adults) and spreads in a manner similar to the common cold: it spreads through saliva and mucus particles that remain in the air after sneezing or coughing or by being left on surfaces.
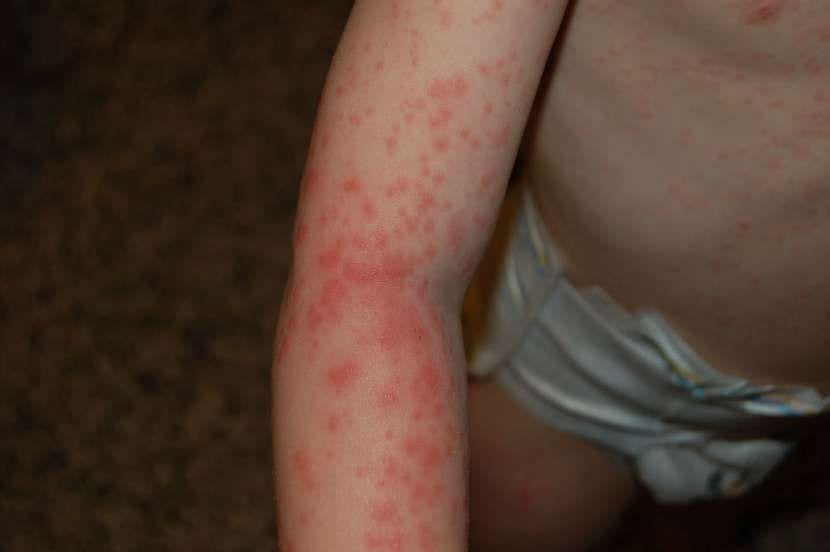
Skin rash is the most prominent symptom of scarlet fever. It usually causes itching or discomfort and starts in the neck and face area, then spreads to the chest, back, and other parts of the body. The skin may feel rough like sandpaper and in many children, the area around the mouth remains paler, which highlights the redness in the cheeks.
These symptoms are accompanied by swelling and irritation in the neck, severe sore throat, and high fever (usually above 38 ºC). The tonsils and the back of the throat are often covered with a whitish coating and show purulent white or yellow spots.
Other common symptoms of this disease include chills, joint pain, nausea, vomiting, and loss of appetite. Since it is a bacterial disease, treatment requires antibiotics; penicillin derivatives are commonly used and should be administered for at least 10 days. During this time, the child needs rest at home and should avoid close contact with other children; complete rest is recommended in the first days of treatment to accelerate the recovery process and reduce the risk of transmission.
The above is a brief introduction to scarlet fever; now we will provide more in-depth information about what it is, how it spreads, what symptoms it shows, how it is treated, and possible complications for both children and adults.
What is Scarlet Fever?
Scarlet fever is an infection caused by the Streptococcus pyogenes bacteria and is also known as group A streptococcus. This bacterium is responsible for the well-known strep throat infection (sore throat, inflammation, and pain) and produces a toxin that triggers the characteristic red rash on the skin in some cases.
In many children, scarlet fever occurs after a strep throat infection. It initially presents with sore throat, fever, and general discomfort, and shortly after, a rash (sarpullido) appears. The rash and fever are the most prominent signs that suggest this disease; there is also a appearance of the tongue known as “strawberry tongue” or “raspberry tongue”, which is very red and filled with swollen papillae.
Scarlet fever was considered a very serious childhood illness in the days before antibiotics and was a significant cause of heart and kidney complications. Today, thanks to early diagnosis and appropriate antibiotic treatment, most cases are mild and improve within a few days; however, outbreaks can still occur in schools and daycare centers.
Currently, cases of scarlet fever have decreased compared to past periods; however, strep throat infections are still common, especially among school-aged children. Importantly, there is no specific vaccine for scarlet fever; thus, measures are primarily based on hygiene practices and infection control.
How Does Scarlet Fever Spread?
The bacteria that cause scarlet fever live in people's noses, throats, and sometimes on their skin. These bacteria spread through saliva and respiratory droplets released when an infected person coughs, sneezes, or talks. These tiny droplets can be directly inhaled or left on surfaces and objects.
The mode of transmission is similar to that of a common cold. If an infected person touches their nose, mouth, or eyes and then touches someone else, or if tableware, glasses, toys, or towels are shared, bacteria can be passed from one person to another. Therefore, in environments where many children are present indoors, such as nurseries and schools, outbreaks of scarlet fever can easily occur.
The most common ways of transmission are as follows:
- Inhaling saliva droplets released during coughing or sneezing.
- Touching contaminated surfaces (toys, tables, doorknobs) and then bringing your hand to your mouth, nose, or eyes.
- Sharing plates, forks, or glasses with someone who carries the bacteria.
- Consuming food prepared by someone who does not follow hygiene rules.
The incubation period for scarlet fever is usually between 2 to 5 days. During this time, a person may not show symptoms or may feel mild discomfort, making it difficult to detect and prevent transmission in the early stages.
Children who have had scarlet fever generally develop a specific immunity to that toxin, so the typical rash is unlikely to recur. However, they can still contract strep throat.
In adults, transmission is usually seen in those who live or work with children, especially in schools, nurseries, or at home. Parents, teachers, and school staff may become infected if they do not have prior immunity or if their immune system is weak.
What Are the Symptoms of Scarlet Fever?
Scarlet fever usually follows a strep throat infection. The first symptoms typically include sudden high fever, severe sore throat, and a general feeling of discomfort. Within one or two days, small red rashes begin to appear; these may be raised and painful or itchy.
The rash usually starts on the chest and abdomen and then spreads to the neck, back, arms, legs, and even the genital area. The skin feels rough and coarse. In most cases, a paler area around the mouth and a noticeable redness in the skin folds (armpits, elbows, groin) can be observed.
The rash typically lasts between two to seven days. As it fades, the skin begins to peel, especially at the fingertips of the hands and feet and in other areas where the rash is more intense.
Other common symptoms of scarlet fever include:
- Chills and a severe feeling of cold.
- Variable intensity of headache.
- Sore throat with white and yellow spots.
- Swelling of the tonsils and difficulty swallowing.
- Nausea and vomiting, especially in young children.
- Swollen and painful lymph nodes in the back of the neck.
- Paler areas around the mouth and neck.
- White and red spots on the tongue, which later becomes very red (strawberry tongue).
- Severe fatigue and general discomfort throughout the body.
In adults, symptoms may be somewhat milder, but still include sore throat, fever, rash, and strawberry tongue. Not all symptoms may appear at the same time, and in some cases, the fever may not be prominent or may even be absent, but the typical rash may still be present.
A doctor confirms the diagnosis of scarlet fever through a physical examination and, in most cases, performs a rapid strep test or throat culture. Once the diagnosis is confirmed, antibiotic treatment is initiated to stop the infection and reduce the risk of complications.
Diagnosis of Scarlet Fever
When encountering a child or adult with a high fever, sore throat, and red rash, a pediatrician or family doctor suspects scarlet fever. To confirm the diagnosis, various tests may be conducted in addition to examining the skin, throat, and lymph nodes in the neck.
The most common tests are:
- Rapid streptococcal test: A sample is taken from the back of the throat using a cotton swab. It provides information within a few minutes about whether group A streptococcus is present. It is a very useful test in the office.
- Throat swab culture: This is also done with a cotton swab, but the sample is sent to the laboratory. It takes longer to get results, but it is more sensitive and can be used to confirm the diagnosis in cases where the rapid test is negative.
The diagnosis should always be made individually by a health professional; because there are other viral diseases (chickenpox, measles, or other viral infections) that can cause fever and rash, and these are not treated with antibiotics. Treating without confirmation can encourage the misuse of antibiotics and may lead to an increase in bacterial resistance.
In severe cases or if complications are suspected, the doctor may request blood tests or other additional tests to assess the child's overall condition and check whether internal organs are affected.
Treatment for Scarlet Fever
When a child is diagnosed with scarlet fever, doctors immediately prescribe antibiotics. These medications help the immune system fight the bacteria causing the infection better, shorten the duration of contagion, and reduce the risk of long-term complications.
Typically, penicillin or amoxicillin is prescribed orally for about 10 days. In certain situations, such as penicillin allergy, appropriate alternative antibiotics are used. Completing the treatment is very important; even if the child feels better within a few days, it is essential to ensure the complete eradication of the bacteria without skipping doses or stopping early.
To alleviate symptoms, the doctor may recommend:
- Ibuprofen or paracetamol to reduce fever and alleviate body aches.
- Pain relievers or special sprays to ease sore throat pain.
- Gargling with mild saline solution or lemon water for children old enough to safely do so to relieve throat irritation.
- Using a cold air humidifier in the room to keep the environment moist and reduce discomfort while breathing.
Additionally, offering the child warm and soft foods (puree, yogurt, soups) that won't irritate the throat, as well as cold foods or drinks like ice cream or frozen fruit, can provide local relief.
Staying hydrated is crucial, especially to prevent dehydration in cases of high fever and vomiting. Rest and sleep help the body recover and allow the immune system to respond better.
Children with scarlet fever should not attend school or daycare as long as they have a fever and for at least 24-48 hours after starting antibiotic treatment; during this time, the risk of contagion significantly decreases. It is best to avoid social activities and close contact with other children during this period.
Can There Be Complications from Scarlet Fever?
In most cases, the rash and other symptoms of scarlet fever disappear within about two weeks and do not leave a lasting effect. However, as with many other infectious diseases, if not treated properly, it can lead to significant complications.
Possible complications include:
- Local infections, otitis media (ear infection), sinusitis, or skin infections.
- Pneumonia or deeper respiratory infections.
- Inflammation of the lymph nodes in the neck, which can lead to pain and noticeable swelling.
- Peritonsillar abscess (accumulation of pus next to the tonsils), which causes severe pain and difficulty opening the mouth.
- Glomerulonephritis, inflammation of the kidney filters that can occur weeks after an infection.
- Rheumatic fever, an inflammatory disease that can affect the heart, joints, brain, or skin, resulting from an abnormal immune response to streptococcus.
- Arthritis, meaning painful inflammation in the joints.
- Osteomyelitis (bone infection), a rare but defined complication.
These complications are currently very rare due to antibiotic use; however, it is important to follow the treatment as recommended by the doctor and to return to the doctor if the child does not improve or worsens.
For pregnant women, scarlet fever does not pose an additional risk to the fetus. The most important thing is to keep symptoms under control and to ensure that the antibiotic treatment used is safe during pregnancy; this will be assessed individually by a healthcare professional.
Prevention and Home Care for Scarlet Fever
Scarlet fever is a contagious disease, but the likelihood of transmission can be significantly reduced by adhering to a series of hygiene and precautionary measures, especially for school-aged children and those living with them.
The main recommendations are as follows:
- Washing hands frequently with water and soap for at least 20 seconds, especially after wiping the nose, coughing, sneezing, or changing diapers.
- Using alcohol-based hand sanitizer when soap and water are not available.
- Covering the mouth and nose with the elbow or a disposable tissue when coughing or sneezing.
- Not sharing tableware, glasses, or bottles with sick individuals.
- At home, keeping the sick child's dishes and toothbrushes separate and washing them carefully after each use.
- Teaching children not to touch their mouths, noses, or eyes after touching shared surfaces or playing with other children.
After 24-48 hours of starting antibiotic treatment, most people stop being contagious; however, it is recommended that the child continue to rest at home until they truly feel better and are fever-free.
At home, in addition to the treatment prescribed by the doctor, things that can help the child's well-being include:
- Offering cold or warm drinks and easy-to-swallow foods.
- Providing a calm and comfortable environment to facilitate the child's rest.
- Monitoring body temperature and administering recommended fever reducers.
- If difficulty breathing, severe pain, neck stiffness, or any concerning symptoms arise, returning to a healthcare professional.
Scarlet fever or “scarlet fever” is considered a rare and mostly mild illness today; however, it requires prompt medical intervention to prevent its spread and minimize the risk of complications. With good information, consistent hygiene measures, and adherence to the pediatrician's or family doctor's instructions, families can manage this infection much more peacefully.
Knowing how it spreads, its typical symptoms, and what to do in case of suspected scarlet fever gives parents and caregivers the opportunity to act in a timely manner, protect the family, and provide better support to the child during the recovery process.







































Comments
(0 Comments)